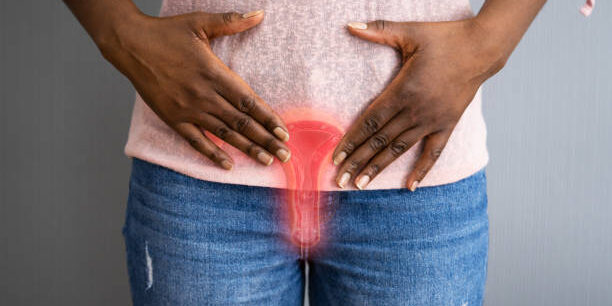
Can I Have Sex With A Urinary Tract Infection (UTI)
Can you have sex with a UTI? is likely the burning question on your mind if you have a urinary tract infection.
It insensible to consider the different ways a UTI may ruin your sex life from now until recovery, even if you aren’t itching to have sex while your symptoms are still creating havoc below.
Can you have sex while taking antibiotics, for instance? When your symptoms have subsided, are you ready to go?
Can you get another UTI when you’re still recuperating from the previous one? The list continues.
Here is a detailed article on everything you need to know if you have questions about any of the above mentionedtopics and are making decisions about your sex life while managing a UTI.

Before we begin, let’s take a look at a few UTI FAQs
I’ll assure you that everything is vital since knowing the fundamentals of UTIs is essential to make wise choicesaround UTI sex.
Additionally, UTIs are rather prevalent, so it’s beneficial to have knowledge of them in your(mental) back pocket.
According to the National Institute of Diabetes and Digestive and Kidney Diseases (NIDDK),between 40 and 60 percent of women who have a vagina will eventually get a UTI.
Read also: Tighten Your Vagina Faster With Kegel Exercises
What exactly is a UTI, again?
Any infection in your urinary system is referred to as a UTI. Your urinary system is madeup of your kidneys, ureter, bladder, and urethra, which is the tube through which you urinate.
Although a UTI canoccur anywhere, it usually occurs when bacteria from your gastrointestinal system migrates from your anus to yourbladder causing cystitis or urethritis.
According to the Merck Manual, UTIs are “ascending infections,” meaning the bacterium maintains an upwardtrajectory for as long as it can until medications eradicate the illness.
If left unattended, germs can spread from yourlower urinary tract to your kidneys, where it may result in sepsis, a potentially fatal illness, or irreversible kidneydamage.
Speaking about UTI classifications, there are two crucial distinctions between simple and complex UTIs.
An uncomplicated UTI is essentially a simple infection that hasn’t damaged your kidneys, isn’t recurring (meaning youdon’t acquire two or more in a six-month period or four or more inside a year), and doesn’t have any other intricate characteristics that might make it more challenging to treat.
How do you know you have a UTI?
Even while UTIs frequently have symptoms, they don’t always manifest on time. The following are a few of themost prevalent signs that let you know you have one.
- A regular urge to urinate
- Burning pee
- Urinating often but in tiny amounts
- Cloudy urine
- Red, bright pink, or brown-colored urine
- Pee that smells strongly
- Your pelvic area hurts, especially in the middle
An infection in your urethra or ureters can cause a burning sensation when youurinate, along with abnormal discharge and hazy urine.
In your bladder it might result in pelvic pressure, lower-abdominal pain, uncomfortable, frequent urination, and blood in your urine.
Additionally, you may have upper backand side discomfort, a high temperature, chills and trembling, nausea, and vomiting if the infection progresses toyour kidneys.
If you are feeling any of these symptoms, please see a doctor immediately.

So what causes a UTI?
I’ll just say it once: bacteria. UTIs develop when germs enter your urinary tract through your urethra.
As wepreviously discussed, this often occurs when bacteria from your gastrointestinal tract enters your bladder.
Sadly, having a vagina increases your risk of developing a UTI.
This is due to two purely anatomical factors:
The proximity of the urethra and anus, and the shorter urethral opening in vaginas compared to penises.
Bacteria don’thave to travel far to trigger problems in your urinary system when you have sex or make the terrible but simple mistake of wiping back to front.
Herpes, gonorrhea, chlamydia, or mycoplasma are examples of sexually transmitteddiseases that can cause germs to enter your urethra and result in urethritis.
However, other risk factors, such as menopause, also increase the occurrence of UTIs in women. These infectionsmay be made worse by estrogen reductions brought on by menopause.
A higher risk of developing UTIs isassociated with uncontrolled diabetes and other immune-suppressing conditions.
Okay, now that you know all there is to know about sex and UTIs.
How do you know whether you can have sex with a UTI?
You’ll have to pardon me for being blunt here, but it relies on a few things. To begin with, I can confirm that, insome cases, it is okay to have sex while suffering from a UTI.
But before you leave, let’s get down to the details.
You must visit the doctor, get a UTI confirmed, and begin treatment before you may consider engaging in sexualactivity.
Whether it involves sex or not, you ought to do this.
UTIs don’t just go away on their own, as we previously stated,therefore getting them treated is your first priority to avoid any potentially harmful side effects.
Your gynecologist’streatment method will be heavily influenced by the type of bacteria causing the illness and whether or not it iscomplex once they have established through tests that you have a UTI.
If your UTI is not problematic, your doctor will recommend an oral antibiotic.
Depending on your unique circumstances, your doctor may advise a different course of treatment if you havestubborn or recurrent UTIs.
This might involve taking low-dose antibiotics for six months or longer, or taking asingle dosage antibiotic just after having intercourse.
Regardless of how frequently you have UTIs, if the infection appears to have progressed to your kidneys, you may need to visit a specialist or go to the hospital where they can give you powerful medicines to fight the infection.
After starting treatment, you can probably have sex, but you should hold off until your symptoms go away.
However, for this to be a smart option, your symptoms truly need to be gone, since sexual activity could only aggravate the region worse.
If you have UTI symptoms, you probably won’t even want to have sex. Not exactly a turn-on when you feel the need to race to the closest restroom every other second.
Even if your symptoms go away, take your antibiotics until the end of the recommended course.
The infection may still be present even though your symptoms have subsided. It might be challenging to predictwhen your UTI will finish.
This is why it’s always important to take the recommended prescription in its entirety.
It will ensure that you truly get rid of the infection rather than merely treating the symptoms, and if you decide toproceed with sex, it will reduce the likelihood that you’ll develop another UTI.
Yes, you read that correctly. Although it is theoretically possible to get a second UTI while recuperating from thefirst, taking medicine to treat your present UTI significantly reduces the likelihood.
If you have an antibiotic onhand, it will probably kill any prospective pathogens that could be considering entering.
Read also: 4 Hidden Locations For The Best Sex Of Your Life
Some good news: It’s unlikely that your birth control will be affected by your UTI medications.
Last but not least, you probably don’t have to be concerned about your UTI medicines interfering with your birth control.
It is true that some antibiotics, such as rifampin (used to treat TB) and griseofulvin (used to treat fungalinfections), have been demonstrated to reduce the effectiveness of hormonal contraception, but there isn’t anyconclusive proof that common UTI medications would have the same effect.
That being said, it wouldn’t hurt toinquire with your doctor or pharmacist about the specific antibiotic you’ve been prescribed to see if there are anylimitations with the birth control method of your choice.
And if you’re truly worried, you may either put off havingsex completely or use a backup form of birth control.
So, yes, if you’re taking antibiotics as directed for your UTI and the symptoms have left your body, you may havesex while still on antibiotics.
However, if you want to be sure, you may always check with your doctor and remember to use a condom.
Also keep in mind that there are steps you may take to avoid developing a UTI in the future.
After experiencing your first UTI, you’ll probably want to stay away from them at all costs in the future.
Use the following products to treat any UTI’s you have

Aday Kit
Get Aday Kit for stubborn vaginal infections
Estriol Vaginal Cream
The following actions can be taken to lower your risk of UTIs:
- Keep hydrated: Drinking enough of fluids, particularly water, can help prevent UTIs. The cause is that you’ll need to urinate more frequently, which makes it more likely that bacteria will be expelled from your urinary system.
- Make sure you’re wiping from front to back as you thoroughly clean. By doing this, you can lessen the risk ofurethral and vaginal infection from anal bacteria.
- After sexual contact, urinate to help wash out any germs that could have colonized the area surrounding your urethra.
- Avoid using anything perfumed there since it might irritate your genitals and urethra, including tampons anddouches (which, by the way, you don’t need).
- Change your birth control technique if you can: Some birth control methods, such diaphragms or condoms coatedwith spermicide, may increase your risk of developing a UTI due to the way they alter your vaginal flora.